Peritoneal Dialysis

For patients with kidney failure (also called end stage renal disease), dialysis is a critical part of care. At this point, the kidneys can no longer fully function on their own, and they need help filtering the blood and removing fluids and waste products.
Generally, there are two types of dialysis. Hemodialysis involves removing blood from the body. Blood flows into a special machine that filters it. Then, the clean blood is returned to the body.
Peritoneal dialysis is different. With this type, blood does not leave the body at all. Instead, the lining of a person’s abdomen (called the peritoneum) cleans the blood and removes fluids and waste.
This article focuses on peritoneal dialysis. More information about hemodialysis is available here.)
What is the peritoneum?
The peritoneum protects abdominal organs
The word peritoneal comes from the word peritoneum. The peritoneum is a membrane found in the abdomen.
The peritoneum has two layers:
- The parietal layer lines the inside wall of the abdominal and pelvic cavities (together called the abdominopelvic cavity.)
- The visceral layer surrounds abdominal organs, including the intestines, stomach, and liver.
The space between these two layers is called the peritoneal cavity.
The peritoneum protects abdominal organs and contains ligaments that keep the organs connected to each other and to the abdominal wall. The peritoneum also filters fluids and wastes, making it a helpful tool for dialysis.
During peritoneal dialysis, a cleansing fluid called dialysate fills the peritoneal cavity. Dialysate contains dextrose, a type of sugar that helps filter the blood.
How does peritoneal dialysis work?
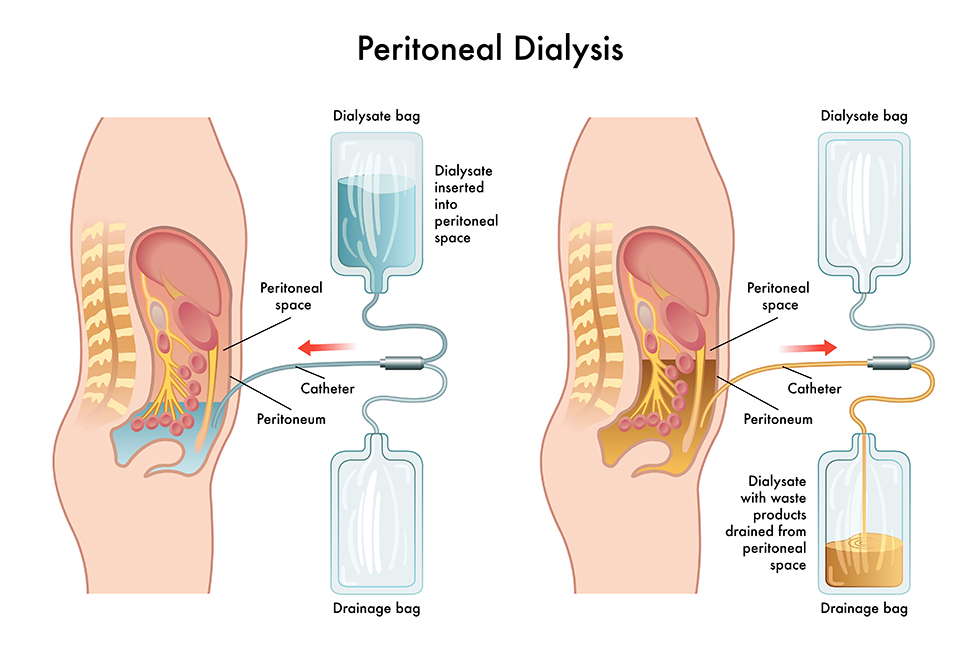
The key to peritoneal dialysis is the exchange. During an exchange, dialysate flows from a sterile plastic bag, through a tube, and into the peritoneal cavity. The dialysate stays in the peritoneal cavity for a prescribed period of time (usually a few hours).
During this time, the dialysate flows around the abdominal organs and makes contact with the peritoneum. The peritoneum acts as a filtering membrane between the blood and the dialysate. Extra fluids and waste products move from the blood, through the peritoneum, to the dialysate. But important substances, like red blood cells and nutrients, do not pass through the peritoneum. They remain in the blood.
Then, the dialysate is drained out of the peritoneal cavity and replaced with new solution.
People do several exchanges during the course of a day. They are given detailed training for this process. A friend or family member can also be trained so that they can help out when necessary.
Peritoneal dialysis can be done almost anywhere, including at home, at work, and while traveling. Patients may need to adjust their activities a bit, but many people find this method to be a convenient alternative to hemodialysis.
Peritoneal dialysis can be done almost anywhere, including at home, at work, and while traveling
Types of peritoneal dialysis
Peritoneal dialysis is categorized in two ways, depending on how the exchanges are done:
- Continuous ambulatory peritoneal dialysis (CAPD). Exchanges are done by hand, without the use of a machine.
- Automated peritoneal dialysis (APD). A machine called a cycler does exchanges at night while a person sleeps.
People who have APD are still trained to do their exchanges by hand.
Getting a catheter
Before either type of dialysis begins, a permanent catheter is placed in the peritoneal cavity. The catheter is a soft tube that provides a pathway for the dialysate to flow in and out of the body. Usually, this surgery happens a few weeks before dialysis starts so that the area has time to fully heal.
During the procedure, the surgeon makes a small opening near the navel (belly button). The catheter is placed through this opening so that one end remains in the peritoneal cavity. The other end sticks out of the belly and is capped at the end. During an exchange, the cap is removed and tubes are connected to insert or drain dialysate.
Patients are placed under general or local anesthesia for this surgery. They may need to say overnight in the hospital.
Peritoneal dialysis training
Before people start doing peritoneal dialysis on their own, they go through several weeks of extensive training with a dialysis nurse. They may also have a friend or family member go through training with them.
During training, patients and their helpers learn how to:
- Prepare for an exchange. This might involve warming up the bag of dialysate in the microwave and opening a set of tubing.
- Connect the bag of dialysate, the tubing, and the catheter.
- Discard used dialysate.
- Program and troubleshoot the cycler, if one is being used.
- Care for the catheter site and keep it clean.
- Lower the risk of infection.
- Order supplies.
Performing CAPD exchanges
Patients are given instructions specific to their situation and equipment. However, the general procedure is as follows:
- Wash hands and put on a surgical mask.
- Use tubing to connect the catheter with a bag of dialysate.
- Allow the prescribed amount of fresh dialysate to flow into the peritoneal cavity. Usually, the amount is two to three quarts.
- Place the cap on the catheter to avoid leaks.
At this point, the peritoneum does its work, filtering wastes from the blood into the dialysate. This dwell time takes several hours. Most people go about their daily activities during this time.
After the dwell time, the used dialysate is drained into an empty bag and discarded. The process repeats with a fresh bag of dialysate.
This process is repeated three to four times a day. The process of draining the peritoneal cavity after the dwell time and refilling it with fresh dialysate takes about 30 minutes.
Performing APD exchanges
APD exchanges work in a similar way, except a machine called a cycler automatically performs the exchanges while a person sleeps. The catheter is connected to the cycler, which is programmed to release a prescribed amount of dialysate into the peritoneal cavity. When the dwell time is finished, the cycler drains the used fluid into a collection container. (Some cycler models drain into a nearby bathtub or toilet.)
What to watch for
Peritoneal dialysis is safe, but patients should know about possible complications:
Peritonitis
Peritonitis is inflammation of the peritoneum, the lining of the abdomen, which filters waste during peritoneal dialysis. If bacteria or fungi reach the peritoneum, an infection can develop.
Symptoms of peritonitis include pain or tenderness in the belly, bloating, fever, nausea, vomiting, and cloudy dialysate after draining.
Peritonitis can be serious. People who have these symptoms should call their doctor immediately. The condition is treated with antibiotics, which may be mixed with the dialysate or given through an IV.
Hernia
Abdominal muscles may weaken from the weight of the dialysate. This situation may cause a hernia.
Weight gain
Dialysate contains dextrose, a type of sugar. The body can absorb extra calories from dextrose, which may cause a person to gain weight, especially if there is a long dwell time. Adjusting the schedule of exchanges might help.
Following up with the doctor
Patients undergoing peritoneal dialysis have regular checkups with their healthcare team. Through lab tests, doctors can assess how well the process is working and whether any adjustments need to be made.
Patients may need to make dietary changes as well. Often, people need to pay close attention to what they eat and drink. They may be advised to limit sodium and phosphorus or increase protein in their diet. Doctors and dietitians can help patients develop a meal plan that works for their lifestyle.
Resources
National Institute of Diabetes and Digestive and Kidney Diseases
“Peritoneal Dialysis”
(Last reviewed: January 2018)
https://www.niddk.nih.gov/health-information/kidney-disease/kidney-failure/peritoneal-dialysis
National Kidney Foundation
“Living Well With Kidney Failure, Part 4: Peritoneal Dialysis”
(Video. Uploaded: January 1, 2009)
https://www.youtube.com/watch?v=kBX4bD10MXM&t=124s
“Peritoneal Dialysis”
(Date Reviewed: June 1, 2021)
https://www.kidney.org/atoz/content/peritoneal
“Peritonitis”
https://www.kidney.org/atoz/content/peritonitis
“Ultrafiltration”
https://www.kidney.org/atoz/content/ultrafiltration
Cleveland Clinic
“Peritoneum”
(Last reviewed: April 27, 2022)
https://my.clevelandclinic.org/health/body/22894-peritoneum
Kenhub.com
Vasković, Jana, MD
“Peritoneum and peritoneal cavity”
(Last reviewed: April 12, 2023)
https://www.kenhub.com/en/library/anatomy/the-peritoneum
Mayo Clinic
“Peritoneal Dialysis”
(May 2, 2023)
https://www.mayoclinic.org/tests-procedures/peritoneal-dialysis/about/pac-20384725

